
| Size | Price | Stock | Qty |
|---|---|---|---|
| 25mg |
|
||
| 50mg |
|
||
| 100mg |
|
||
| 250mg |
|
||
| 500mg |
|
||
| 1g |
|
||
| 2g | |||
| Other Sizes |
Purity: ≥98%
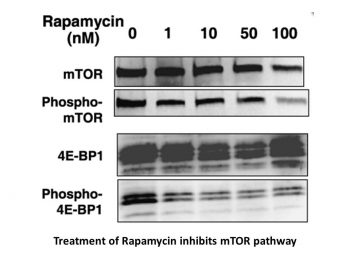
Rapamycin (also known as Sirolimus; AY-22989), a natural macrocyclic lactone isolated from the bacterium Streptomyces hygroscopicus, is a specific and potent mTOR inhibitor with IC50 of ~0.1 nM in HEK293 cells. Although rapamycin was initially created as an antifungal antibiotic, it also showed signs of immunosuppressive activity, and it is now used for this reason to prevent transplant rejection. Additionally, it shows activity against a number of transplantable tumors and is only marginally to completely inactive against leukemias. Rapamycin suppresses the immune system by preventing T cells from activating and proliferating. The rapamycin-FKBP12 complex, which is formed when rapamycin binds to FK-binding protein 12 (FKBP12), controls an enzyme that is crucial to the progression of the cell cycle.
| Targets |
mTOR (IC50 = 0.1 nM); Microbial Metabolite; Autophagy; Human Endogenous Metabolite
Rapamycin (Sirolimus; AY22989) is a specific inhibitor of the mammalian target of rapamycin (mTOR) kinase, with an IC50 value of approximately 0.1-0.5 nM for mTORC1 inhibition [1][3][4]. |
|---|---|
| ln Vitro |
Rapamycin (Sirolimus; AY22989) inhibits endogenous mTOR activity in HEK293 cells with IC50 of ~0.1 nM, more potently than iRap and AP21967 with IC50 of ~5 nM and ~10 nM, respectively. [1] Rapamycin treatment causes a severe G1/S cell cycle arrest in Saccharomyces cerevisiae and inhibits translation initiation to levels below 20% of control. [2] Rapamycin exhibits little activity against U373-MG cells with an IC50 of >25 M despite having a similar impact on the inhibition of mTOR signaling. Rapamycin significantly reduces the cell viability of T98G and U87-MG in a dose-dependent manner. By inhibiting the activity of mTOR, rapamycin (100 nM) causes G1 arrest and autophagy but not apoptosis in Rapamycin-sensitive U87-MG and T98G cells. [3]
Saccharomyces cerevisiae cells treated with the immunosuppressant Rapamycin (Sirolimus; AY22989) or depleted for the targets of rapamycin TOR1 and TOR2 arrest growth in the early G1 phase of the cell cycle. Loss of TOR function also causes an early inhibition of translation initiation and induces several other physiological changes characteristic of starved cells entering stationary phase (G0). A G1 cyclin mRNA whose translational control is altered by substitution of the UBI4 5' leader region (UBI4 is normally translated under starvation conditions) suppresses the rapamycin-induced G1 arrest and confers starvation sensitivity. These results suggest that the block in translation initiation is a direct consequence of loss of TOR function and the cause of the G1 arrest. We propose that the TORs, two related phosphatidylinositol kinase homologues, are part of a novel signaling pathway that activates eIF-4E-dependent protein synthesis and, thereby, G1 progression in response to nutrient availability. Such a pathway may constitute a checkpoint that prevents early G1 progression and growth in the absence of nutrients. [2] The mammalian target of rapamycin (mTOR) is a downstream effector of the phosphatidylinositol 3-kinase (PI3K)/protein kinase B (Akt) signaling pathway and a central modulator of cell proliferation in malignant gliomas. Therefore, the targeting of mTOR signaling is considered a promising therapy for malignant gliomas. However, the mechanisms underlying the cytotoxic effects of a selective mTOR inhibitor, Rapamycin (Sirolimus; AY22989), on malignant glioma cells are poorly understood. The purpose of this study was thus to elucidate how rapamycin exerts its cytotoxic effects on malignant glioma cells. We showed that rapamycin induced autophagy but not apoptosis in rapamycin-sensitive malignant glioma U87-MG and T98G cells by inhibiting the function of mTOR. In contrast, in rapamycin-resistant U373-MG cells, the inhibitory effect of rapamycin was minor, although the phosphorylation of p70S6 kinase, a molecule downstream of mTOR, was remarkably inhibited. Interestingly, a PI3K inhibitor, LY294002, and an Akt inhibitor, UCN-01 (7-hydroxystaurosporine), both synergistically sensitized U87-MG and T98G cells as well as U373-MG cells to rapamycin by stimulating the induction of autophagy. Enforced expression of active Akt in tumor cells suppressed the combined effects of LY294002 or UCN-01, whereas dominant-negative Akt expression was sufficient to increase the sensitivity of tumor cells to rapamycin. These results indicate that rapamycin exerts its antitumor effect on malignant glioma cells by inducing autophagy and suggest that in malignant glioma cells a disruption of the PI3K/Akt signaling pathway could greatly enhance the effectiveness of mTOR inhibitors. [3] - Autophagy Induction in Glioma Cells: In malignant glioma cell lines (e.g., U87-MG), Rapamycin (10 nM) induced autophagy as evidenced by increased LC3-II protein levels and formation of autophagosomes. Co-treatment with phosphatidylinositol 3-kinase (PI3K) inhibitors (e.g., LY294002, 10 μM) synergistically enhanced rapamycin-induced autophagy, leading to a significant reduction in cell viability compared to single-agent treatment [3]. - mTORC1 Inhibition: Rapamycin (0.1-10 nM) potently inhibited mTORC1 activity in vitro, as demonstrated by decreased phosphorylation of downstream targets such as S6K1 and 4E-BP1 in various cell types [1][3][4]. |
| ln Vivo |
Treatment with Rapamycin (Sirolimus; AY22989) in vivo specifically blocks targets known to be downstream of mTOR such as the phosphorylation and activation of p70S6K and the release of inhibition of eIF4E by PHAS-1/4E-BP1, leading to complete blockage of the hypertrophic increases in plantaris muscle weight and fibre size.[4] Short-term Rapamycin treatment, even at the lowest dose of 0.16 mg/kg, results in profound inhibition of p70S6K activity, which is correlated with an increase in tumor cell death and necrosis of the Eker renal tumors. [5] By lowering VEGF production and preventing VEGF-induced endothelial cell signaling, rapamycin inhibits angiogenesis and metastatic tumor growth in CT-26 xenograft models. [6] Rapamycin treatment at 4 mg/kg/day significantly reduces tumor vascular permeability and tumor growth in C6 xenografts. [7]
Skeletal muscles adapt to changes in their workload by regulating fibre size by unknown mechanisms. The roles of two signalling pathways implicated in muscle hypertrophy on the basis of findings in vitro, Akt/mTOR (mammalian target of rapamycin) and calcineurin/NFAT (nuclear factor of activated T cells), were investigated in several models of skeletal muscle hypertrophy and atrophy in vivo. The Akt/mTOR pathway was upregulated during hypertrophy and downregulated during muscle atrophy. Furthermore, rapamycin, a selective blocker of mTOR, blocked hypertrophy in all models tested, without causing atrophy in control muscles. In contrast, the calcineurin pathway was not activated during hypertrophy in vivo, and inhibitors of calcineurin, cyclosporin A and FK506 did not blunt hypertrophy. Finally, genetic activation of the Akt/mTOR pathway was sufficient to cause hypertrophy and prevent atrophy in vivo, whereas genetic blockade of this pathway blocked hypertrophy in vivo. We conclude that the activation of the Akt/mTOR pathway and its downstream targets, p70S6K and PHAS-1/4E-BP1, is requisitely involved in regulating skeletal muscle fibre size, and that activation of the Akt/mTOR pathway can oppose muscle atrophy induced by disuse. Muscle Atrophy Prevention in Mice: In a mouse model of hindlimb unloading-induced muscle atrophy, Rapamycin (1 mg/kg/day, intraperitoneal injection) for 14 days significantly prevented muscle wasting. The tibialis anterior and gastrocnemius muscles in treated mice showed 20-30% higher weight and 15-25% larger cross-sectional area compared to vehicle-treated controls. Additionally, the expression of atrophy-related genes (Atrogin-1 and MuRF-1) was reduced by 40-50% in treated muscles [4]. Regulation of Skeletal Muscle Hypertrophy: In mice with IGF-1-induced skeletal muscle hypertrophy, Rapamycin (1 mg/kg/day, intraperitoneal) administration for 7 days inhibited the hypertrophy response, as indicated by a 25-35% reduction in muscle mass gain compared to IGF-1 alone. This was associated with decreased phosphorylation of S6K1 and 4E-BP1 in muscle tissues [4]. |
| Enzyme Assay |
HEK293 cells are plated at 2-2.5×10~5 cells/well of a 12-well plate and serum-starved for 24 hours in DMEM. Rapamycin (Sirolimus; AY22989) (0.05–50 nM) is administered to cells for 15 minutes at 37 °C in escalating concentrations. 30 minutes at 37 °C are spent adding serum at a final concentration of 20%. Cell lysates are separated by SDS-PAGE after being lysed. Proteins that have been resolved are transferred to a polyvinylidene difluoride membrane and immunoblotted using a primary antibody that is phosphospecific for the Thr-389 of p70 S6 kinase. using ImageQuant and KaleidaGr for data analysis.[1]
Rapamycin (Sirolimus; AY22989) is an immunosuppressive drug that binds simultaneously to the 12-kDa FK506- and rapamycin-binding protein (FKBP12, or FKBP) and the FKBP-rapamycin binding (FRB) domain of the mammalian target of rapamycin (mTOR) kinase. The resulting ternary complex has been used to conditionally perturb protein function, and one such method involves perturbation of a protein of interest through its mislocalization. We synthesized two rapamycin derivatives that possess large substituents at the C-16 position within the FRB-binding interface, and these derivatives were screened against a library of FRB mutants using a three-hybrid assay in Saccharomyces cerevisiae. Several FRB mutants responded to one of the rapamycin derivatives, and twenty of these mutants were further characterized in mammalian cells. The mutants most responsive to the ligand were fused to yellow fluorescent protein, and fluorescence levels in the presence and absence of the ligand were measured to determine stability of the fusion proteins. Wild-type and mutant FRB domains were expressed at low levels in the absence of the rapamycin derivative, and expression levels rose up to 10-fold upon treatment with ligand. The synthetic rapamycin derivatives were further analyzed using quantitative mass spectrometry, and one of the compounds was found to contain contaminating rapamycin. Furthermore, uncontaminated analogs retained the ability to inhibit mTOR, although with diminished potency relative to rapamycin. The ligand-dependent stability displayed by wild-type FRB and FRB mutants as well as the inhibitory potential and purity of the rapamycin derivatives should be considered as potentially confounding experimental variables when using these systems. [1] - mTOR Kinase Activity Assay: Recombinant mTOR kinase was incubated with ATP and a synthetic peptide substrate in the presence of Rapamycin (0.01-100 nM). The reaction was terminated by adding SDS-PAGE loading buffer, and phosphorylated products were detected by immunoblotting with phospho-specific antibodies. Rapamycin inhibited mTOR kinase activity with an IC50 of 0.1-0.5 nM [1][3][4]. |
| Cell Assay |
Cells are exposed to various concentrations of Rapamycin (Sirolimus; AY22989) for 72 hours. For the assessment of cell viability, cells are collected by trypsinization, stained with trypan blue, and the viable cells in each well are counted. For the determination of cell cycle, cells are trypsinized, fixed with 70% ethanol, and stained with propidium iodide using a flow cytometry reagent set. Samples are analyzed for DNA content using a FACScan flow cytometer and CellQuest software. For apoptosis detection, cells are stained with the terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling (TUNEL) technique using an ApopTag apoptosis detection kit. To detect the development of acidic vesicular organelles (AVO), cells are stained with acridine orange (1 μg/mL) for 15 minutes, and examined under a fluorescence microscope. To quantify the development of AVOs, cells are stained with acridine orange (1 μg/mL) for 15 minutes, removed from the plate with trypsin-EDTA, and analyzed using the FACScan flow cytometer and CellQuest software. To analyze the autophagic process, cells are incubated for 10 minutes with 0.05 mM monodansylcadaverine at 37 °C and are then observed under a fluorescence microscope.
Cell viability assay. To determine the effects of rapamycin and Rapamycin (Sirolimus; AY22989) plus LY294002 or UCN-01 on tumor cells, we determined cell viability after the treatments. We used a trypan blue dye exclusion assay as described previously. Tumor cells in exponential growth were harvested and seeded at 5 × 103 cells per well (0.1 mL) in 96-well flat-bottomed plates and incubated overnight at 37°C. The cells were then incubated for 72 hours with or without rapamycin or with rapamycin plus LY294002 or UCN-01. After the cells were collected by trypsinization, they were stained with trypan blue, and the viable cells in each well were counted. The viability of the untreated cells (the control) was considered 100%. Survival fractions were calculated from the mean cell viability of the treated cells. [3] - Glioma Cell Viability Assay: Malignant glioma cells were treated with Rapamycin (1-100 nM) alone or in combination with PI3K inhibitors (1-10 μM) for 48 hours. Cell viability was assessed using the MTT assay. Rapamycin alone reduced cell viability by 30-50% at 10 nM, while combination treatment resulted in a 60-80% reduction [3]. - Skeletal Muscle Cell Hypertrophy Assay: In C2C12 myoblasts, Rapamycin (10 nM) inhibited insulin-like growth factor 1 (IGF-1)-induced hypertrophy, as indicated by reduced cell size and decreased expression of hypertrophy markers (e.g., MyoD, myogenin) [4]. |
| Animal Protocol |
Athymic Nu/Nu mice inoculated subcutaneously with VEGF-A-expressing C6 rat glioma cells
~4 mg/kg/day Injection i.p. Drug administration in vivo.[4] Animals were randomized to treatment or vehicle groups so that the mean starting body weights of each group were equal. Drug treatment began on the day of surgery or on the first day of reloading after the 14-day suspension. Rapamycin was delivered once daily by intraperitoneal injection at a dose of 1.5 mg kg−1, dissolved in 2% carboxymethylcellulose. CsA was delivered once daily by subcutaneous injection at a dose of 15 mg kg−1, dissolved in 10% methanol and olive oil. FK506 was delivered once daily via subcutaneous injection at a dose of 3 mg kg−1, dissolved in 10% ethanol, 10% cremophor and saline.[4] Muscle Atrophy Prevention in Mice: Rapamycin (1 mg/kg/day, intraperitoneal injection) was administered to mice subjected to hindlimb unloading to induce muscle atrophy. Treatment significantly prevented muscle wasting, as measured by muscle weight and cross-sectional area of tibialis anterior and gastrocnemius muscles. Rapamycin also reduced the expression of atrophy-related genes (e.g., Atrogin-1, MuRF-1) [4]. |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion
In adult kidney transplant patients with low to moderate immune risk, after oral administration of 2 mg sirolimus, the peak plasma concentration (Cmax) was 14.4 ± 5.3 ng/mL for the oral solution and 15.0 ± 4.9 ng/mL for the oral tablets. The time to peak concentration (tmax) was 2.1 ± 0.8 hours for the oral solution and 3.5 ± 2.4 hours for the oral tablets. The time to peak concentration (tmax) in healthy subjects was 1 hour. In a multiple-dose study, with repeated dosing twice daily without an initial loading dose, steady-state plasma concentrations were reached after 6 days, with the mean trough concentration of sirolimus increasing approximately 2 to 3 times. It is speculated that for most patients, a loading dose three times the maintenance dose can achieve near-steady-state plasma concentrations within 1 day. The systemic bioavailability of sirolimus is approximately 14%. In healthy subjects, the mean bioavailability of sirolimus was approximately 27% higher after tablet administration than after solution administration. Sirolimus tablets and solution are not bioequivalent; however, clinical equivalence has been demonstrated at the 2 mg dose level. In stable kidney transplant patients, sirolimus plasma concentrations were dose-proportional in the range of 3 to 12 mg/m² after administration of rapamycin oral solution. Following oral administration of [14C] sirolimus in healthy subjects, approximately 91% of the radioactive material was recovered in feces, and only 2.2% was detectable in urine. Some metabolites of sirolimus were also detectable in feces and urine. In stable kidney transplant patients, the mean (± SD) plasma ratio of sirolimus was 36 ± 18 L, indicating widespread distribution of sirolimus in blood cells. The mean volume of distribution (Vss/F) of sirolimus is 12 ± 8 L/kg. In adult kidney transplant patients with low to moderate immune risk, the clearance of oral solution after 2 mg sirolimus was 173 ± 50 mL/h/kg, and the clearance of oral tablets was 139 ± 63 mL/h/kg. Sirolimus is rapidly absorbed after administration of oral solution; the mean time to peak concentration (tmax) after a single dose in healthy subjects is approximately 1 hour, while the mean time to peak concentration after multiple oral doses in kidney transplant recipients is approximately 2 hours. The systemic bioavailability of sirolimus after administration of oral solution is estimated to be approximately 14%. After administration of tablets, the mean bioavailability of sirolimus is approximately 27% higher than that of oral solution. In 22 healthy volunteers who received oral rapamycin solution, a high-fat meal altered the bioavailability profile of sirolimus. Compared to fasting, a 34% decrease in peak plasma concentration (Cmax), a 3.5-fold increase in time to peak concentration (tmax), and a 35% increase in total exposure (AUC) were observed. In 24 healthy volunteers who took rapamycin tablets and consumed a high-fat meal, Cmax, tmax, and AUC increased by 65%, 32%, and 23%, respectively. Absorption: Rapid, absorbed via the gastrointestinal tract. Bioavailability is approximately 14%. A high-fat diet reduces absorption. Absorption rate and extent are reduced in Black patients. In kidney transplant recipients with stable conditions, the mean (± standard deviation) plasma-to-serotonin ratio of sirolimus was 36±17.9, indicating widespread distribution of sirolimus in blood cell components. The mean volume of distribution of sirolimus is 12±7.52 L/kg. Sirolimus binds highly to human plasma proteins (approximately 92%). In humans, sirolimus binding is primarily associated with serum albumin (97%), α1-acid glycoprotein, and lipoprotein. For more complete data on the absorption, distribution, and excretion of sirolimus (7 items), please visit the HSDB record page. Metabolism/Metabolites Sirolimus is extensively metabolized in the intestinal wall and liver. Sirolimus is primarily metabolized via O-demethylation and/or hydroxylation by CYP3A4, yielding seven major metabolites, including hydroxy, demethyl, and hydroxydemethyl metabolites, which are pharmacologically inactive. Sirolimus can also be retrogradely transported from the small intestine into the intestinal lumen by enterocytes. Sirolimus is a substrate of cytochrome P450 IIIA4 (CYP3A4) and P-glycoprotein. Sirolimus is primarily metabolized via O-demethylation and/or hydroxylation. Seven major metabolites, including hydroxy, demethyl, and hydroxydemethyl metabolites, are detectable in whole blood. Some of these metabolites are also detectable in plasma, fecal, and urine samples. Glucuronide and sulfate conjugates are not present in any biological matrix. Biotransformation: Primarily occurs in the liver, extensively catalyzed by cytochrome P450 3A enzymes. Major metabolites include hydroxysirolimus, desmethylsirolimus, and hydroxydesmethylsirolimus. …After incubation of sirolimus with human and porcine small intestinal microsomes, five metabolites were detected by high-performance liquid chromatography/electrospray ionization mass spectrometry: hydroxysirolimus, dihydroxysirolimus, trihydroxysirolimus, desmethylsirolimus, and bisdesmethylsirolimus. The same metabolites were also produced by human liver microsomes and porcine small intestinal mucosa in the Ussing chamber. Anti-CYP3A antibodies, as well as specific CYP3A inhibitors tromethamine and erythromycin, inhibited the metabolism of sirolimus in the small intestine, confirming that, like in the liver, CYP3A enzymes are responsible for the metabolism of sirolimus in the small intestine. ... The known metabolites of sirolimus include 16-O-desmethylsirolimus, 39-O-desmethylsirolimus, 24-hydroxysirolimus, 11-hydroxysirolimus, 25-hydroxysirolimus, 46-hydroxysirolimus, and 12-hydroxysirolimus. Biological half-life In stable kidney transplant patients, the mean terminal elimination half-life (t½) of sirolimus after multiple doses is estimated to be approximately 62 ± 16 hours. The elimination half-life of this drug in kidney transplant recipients is 57–63 hours. -Oral bioavailability: In preclinical studies, rapamycin had low oral bioavailability (approximately 15–20%) due to extensive first-pass metabolism in the body. Liver and intestines [1][3]. - Half-life: The plasma half-life of rapamycin in mice and rats is approximately 6–12 hours after intravenous injection [1][3]. |
| Toxicity/Toxicokinetics |
Hepatotoxicity
Some patients taking sirolimus may experience elevated serum enzymes, but these abnormalities are usually mild, asymptomatic, and resolve spontaneously, rarely requiring dose adjustment or discontinuation. Sirolimus use has been reported to cause rare cholestatic hepatitis, but the specific characteristics of clinical liver injury caused by this drug are not yet clear. Most published cases of sirolimus-related liver injury occur in patients who have been exposed to other potentially hepatotoxic drugs or have other underlying causes (such as sepsis, cancer, or parenteral nutrition). Patients receiving sirolimus after liver transplantation have been reported to have a higher risk of hepatic artery thrombosis, but this association remains controversial. Probability score: C (likely a rare cause of clinically significant liver injury). Pregnancy and Lactation Effects ◉ Overview of Use During Lactation Because there is little information regarding oral sirolimus during lactation, alternative medications may be preferred, especially in breastfed newborns or premature infants. Sirolimus is undetectable in blood after topical application, therefore, topical application of sirolimus is unlikely to affect breastfed infants. Avoid application to the nipple area and ensure that the infant's skin does not come into direct contact with the treated area. ◉ Effects on breastfed infants An infant was reported to be breastfed (feeding extent not specified) while the mother received treatment with sirolimus, tacrolimus, and prednisone (dosage not specified) after a kidney and pancreas transplant. The authors who followed the mother did not observe any serious side effects in the infant. ◉ Effects on lactation and breast milk No relevant published information was found as of the revision date. Protein binding Sirolimus binds to 92% of human plasma proteins, primarily serum albumin (97%), α1-acid glycoprotein, and lipoprotein. Interactions Since St. John's wort (Hypericum perforatum) can induce the activity of CYP3A4 and P-glycoprotein, and sirolimus is a substrate of both, concomitant administration of St. John's wort and sirolimus may lead to a decrease in sirolimus concentration. /Concomitant use of sirolimus and tacrolimus/ may increase mortality, transplant failure, and hepatic artery thrombosis (HAT) in liver transplant patients, with most HAT occurring within 30 days post-transplantation. /Antibiotics, such as rifabutin or rifapentine; and anticonvulsants, such as carbamazepine, phenobarbital, or phenytoin sodium/ may decrease sirolimus concentration due to induction by the cytochrome P450 3A4 (CYP3A4) isoenzyme. When used in combination with rifampin, sirolimus clearance is significantly increased due to rifampin induction of CYP3A4; alternative antimicrobial agents with lower enzyme induction potential should be considered. For more complete data on interactions of sirolimus (11 in total), please visit the HSDB record page. Non-human toxicity values Intraperitoneal LD50 in mice: 600 mg/kg Oral LD50 in mice: >2,500 mg/kg |
| References |
|
| Additional Infomation |
Therapeutic Uses
Sirolimus is indicated for the prevention of kidney transplant rejection. It is recommended that sirolimus be used in combination with cyclosporine and corticosteroids. /US product label includes/ The long-term efficacy of percutaneous coronary intervention for chronic total coronary occlusion is limited by high restenosis and reocclusion rates. Sirolimus-eluting stents have shown significantly reduced restenosis rates compared to bare-metal stents in treating relatively simple non-occlusive lesions, but whether these results have broader applicability is unclear. The use of sirolimus-eluting stents for chronic total coronary occlusion reduces the incidence of major adverse cardiac events and restenosis compared to bare-metal stents. Chronic renal failure induced by calcineurin inhibitor (CNI) immunosuppression is a common complication after heart transplantation. Sirolimus and mycophenolate mofetil (MMF) are two relatively new immunosuppressants for which no nephrotoxic side effects have been reported. This case report describes a patient with persistent chronic renal failure after 10 months of cyclosporine immunosuppressive therapy. After switching the immunosuppressive regimen from cyclosporine to sirolimus and mycophenolate mofetil (MMF), the patient did not experience acute rejection, had good heart transplant function, and continued improvement in renal function. This case illustrates the potential of sirolimus and mycophenolate mofetil (MMF) as safe, long-term immunosuppressants without calcineurin inhibitors (CNIs) in patients with chronic renal failure after heart transplantation. Drug Warning /Black Box Warning/ Immunosuppressant, not recommended for liver or lung transplant patients. Immunosuppression may increase susceptibility to infection and may lead to lymphoma and other malignancies. Immunosuppression may increase susceptibility to infection and may lead to lymphoma. Rapamycin should only be used by physicians experienced in immunosuppressive therapy and the management of kidney transplant patients. Patients receiving this drug should be treated in a healthcare facility with adequate laboratory and supportive medical resources. The physician responsible for maintenance therapy should have all information necessary for patient follow-up. The safety and efficacy of rapamycin (sirolimus) as an immunosuppressant in liver or lung transplant patients have not been established and therefore it is not recommended for such treatment. Liver Transplantation – Increased Mortality, Graft Loss, and Hepatic Artery Thrombosis (HAT): A study in primary liver transplant recipients showed that rapamycin combined with tacrolimus was associated with increased mortality and graft loss. Many patients had evidence of infection at or around the time of death. In this study, and another study in primary liver transplant recipients, rapamycin combined with cyclosporine or tacrolimus was associated with an increased incidence of HAT; most HAT cases occurred within 30 days post-transplantation, and most resulted in graft loss or death. Lung Transplantation – Bronchial Anastomosis Dehiscence: Cases of bronchial anastomosis dehiscence have been reported in lung transplant recipients when rapamycin was used as part of an immunosuppressive regimen, most of which were fatal. Grapefruit juice may inhibit the CYP3A4 enzyme, leading to decreased sirolimus metabolism; therefore, it should not be taken concurrently with sirolimus or used to dilute sirolimus. In lung transplant recipients, there have been reports of bronchial anastomotic dehiscence when sirolimus is used in combination with other immunosuppressants, most of which were fatal. Because the safety and efficacy of sirolimus as immunosuppressive therapy in lung transplant patients have not been established, the manufacturer does not recommend its use for this purpose. The combination of sirolimus with other immunosuppressants (such as cyclosporine and tacrolimus) increases the risk of hepatic artery thrombosis, graft loss, and death in primary liver transplant recipients. Because the safety and efficacy of sirolimus as immunosuppressive therapy in liver transplant patients have not been established, the manufacturer does not recommend its use for this purpose. For more complete data on sirolimus (27 total), please visit the HSDB record page. Pharmacodynamics Sirolimus is an immunosuppressant with antifungal and antitumor effects. In animal models, sirolimus prolonged allogeneic transplant survival after multiple organ transplants and reversed acute rejection in rat heart and kidney allogeneic transplants. Compared with azathioprine or placebo, daily oral administration of 2 mg and 5 mg sirolimus significantly reduced the incidence of organ rejection in low- to moderate-immune-risk kidney transplant recipients at 6 months post-transplantation. In some studies, the immunosuppressive effect of sirolimus has persisted for up to 6 months after discontinuation: this immune tolerance is allogeneic antigen specific. Sirolimus effectively inhibits antigen-induced T-cell and B-cell proliferation and antibody production. In rodent models of autoimmune diseases, sirolimus inhibited immune-mediated events associated with systemic lupus erythematosus, collagen-induced arthritis, autoimmune type 1 diabetes, autoimmune myocarditis, experimental allergic encephalomyelitis, graft-versus-host disease, and autoimmune uveoretinitis. - Mechanism of action: Rapamycin binds to FKBP12 to form a complex that inhibits mTORC1 by blocking its kinase activity. This leads to inhibition of protein synthesis, induction of autophagy, and inhibition of cell growth and proliferation [1][3][4]. - Clinical applications: Rapamycin has been approved for immunosuppression in organ transplantation and for the treatment of certain cancers. It has also shown promise in preclinical models for the prevention of muscle atrophy and the treatment of neurodegenerative diseases [1][3][4]. - Side effects: Common side effects of rapamycin include immunosuppression, hyperlipidemia, and hyperglycemia. Long-term use may increase the risk of infection and certain cancers [1][3][4]. |
| Molecular Formula |
C51H79NO13
|
|---|---|
| Molecular Weight |
914.18
|
| Exact Mass |
913.555
|
| Elemental Analysis |
C, 67.01; H, 8.71; N, 1.53; O, 22.75
|
| CAS # |
53123-88-9
|
| Related CAS # |
Rapamycin;53123-88-9
|
| PubChem CID |
5284616
|
| Appearance |
White to off-white solid powder
|
| Density |
1.2±0.1 g/cm3
|
| Boiling Point |
973.0±75.0 °C at 760 mmHg
|
| Melting Point |
183-185°C
|
| Flash Point |
542.3±37.1 °C
|
| Vapour Pressure |
0.0±0.6 mmHg at 25°C
|
| Index of Refraction |
1.551
|
| LogP |
3.54
|
| Hydrogen Bond Donor Count |
3
|
| Hydrogen Bond Acceptor Count |
13
|
| Rotatable Bond Count |
6
|
| Heavy Atom Count |
65
|
| Complexity |
1760
|
| Defined Atom Stereocenter Count |
15
|
| SMILES |
O(C([H])([H])[H])[C@@]1([H])[C@@]([H])(C([H])([H])C([H])([H])[C@@]([H])(C([H])([H])[C@@]([H])(C([H])([H])[H])[C@]2([H])C([H])([H])C([C@@]([H])(C([H])=C(C([H])([H])[H])[C@]([H])([C@]([H])(C([C@]([H])(C([H])([H])[H])C([H])([H])[C@]([H])(C([H])([H])[H])C([H])=C([H])C([H])=C([H])C([H])=C(C([H])([H])[H])[C@]([H])(C([H])([H])[C@]3([H])C([H])([H])C([H])([H])[C@@]([H])(C([H])([H])[H])[C@@](C(C(N4C([H])([H])C([H])([H])C([H])([H])C([H])([H])[C@@]4([H])C(=O)O2)=O)=O)(O[H])O3)OC([H])([H])[H])=O)OC([H])([H])[H])O[H])C([H])([H])[H])=O)C1([H])[H])O[H] |c:35,66,70,t:62|
|
| InChi Key |
QFJCIRLUMZQUOT-PYYJPVDBSA-N
|
| InChi Code |
InChI=1S/C51H79NO13/c1-30-16-12-11-13-17-31(2)42(61-8)28-38-21-19-36(7)51(60,65-38)48(57)49(58)52-23-15-14-18-39(52)50(59)64-43(33(4)26-37-20-22-40(53)44(27-37)62-9)29-41(54)32(3)25-35(6)46(56)47(63-10)45(55)34(5)24-30/h11-13,16-17,25,30,32-34,36-40,42-44,46-47,53,56,60H,14-15,18-24,26-29H2,1-10H3/b13-11+,16-12+,31-17+,35-25+/t30-,32-,33-,34-,36-,37+,38+,39+,40-,42+,43+,44?,46-,47+,51-/m1/s1
|
| Chemical Name |
(3S,6R,7E,9R,10R,12R,14S,15E,17E,19E,21S,23S,26R,27R,34aS)-9,10,12,13,14,21,22,23,24,25,26,27,32,33,34, 34a-hexadecahydro-9,27-dihydroxy-3-[(1R)-2-[(1S,3R,4R)-4-hydroxy-3-methoxycyclohexyl]-1-methylethyl]-10,21-dimethoxy-6,8,12,14,20,26-hexamethyl-23,27-epoxy-3H-pyrido[2,1-c][1,4] oxaazacyclohentriacontine-1,5,11,28,29 (4H,6H,31H)-pentone
|
| Synonyms |
AY 22989; AY22989; AY-22989; NSC-2260804; RAPA; RAP; RPM; SLM; AY 22989; SILA 9268A; WY090217; WY-090217; WY 090217; C07909; D00753; I 2190A; I-2190A; I2190A; NSC 226080; Rapamune
|
| HS Tariff Code |
2934.99.9001
|
| Storage |
Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition |
Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs)
|
| Solubility (In Vitro) |
|
|||
|---|---|---|---|---|
| Solubility (In Vivo) |
Formulation 1: 2% DMSO + 30% PEG 300 + 5% Tween 80 + ddH2O: 5 mg/mL; suspension
Formulation 2: 0.5% CMC-Na + 1%Tween-80 in Saline water: 1.98 mg/mL (2.17 mM); suspension Formulation 3: 10% DMSO + 90% Corn Oil: ≥ 2.08 mg/mL (2.28 mM); clear solution Formulation 4: 10% EtOH + 40% PEG300 + 5% Tween-80 + 45% Saline: ≥ 2.5 mg/mL (2.73 mM); suspension Formulation 5: 10% EtOH + 90% (20% SBE-β-CD in Saline): 2.5 mg/mL (2.73 mM); suspension Formulation 6: 10% EtOH + 90% Corn Oil: ≥ 2.5 mg/mL (2.73 mM); suspension Formulation 7: 10% DMSO + 40% PEG300 + 5% Tween-80 + 45% Saline: ≥ 2.08 mg/mL (2.28 mM); clear solution Formulation 8: 10% DMSO + 90% (20% SBE-β-CD in Saline): 2.08 mg/mL (2.28 mM); suspension (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.0939 mL | 5.4694 mL | 10.9388 mL | |
| 5 mM | 0.2188 mL | 1.0939 mL | 2.1878 mL | |
| 10 mM | 0.1094 mL | 0.5469 mL | 1.0939 mL |
*Note: Please select an appropriate solvent for the preparation of stock solution based on your experiment needs. For most products, DMSO can be used for preparing stock solutions (e.g. 5 mM, 10 mM, or 20 mM concentration); some products with high aqueous solubility may be dissolved in water directly. Solubility information is available at the above Solubility Data section. Once the stock solution is prepared, aliquot it to routine usage volumes and store at -20°C or -80°C. Avoid repeated freeze and thaw cycles.
Calculation results
Working concentration: mg/mL;
Method for preparing DMSO stock solution: mg drug pre-dissolved in μL DMSO (stock solution concentration mg/mL). Please contact us first if the concentration exceeds the DMSO solubility of the batch of drug.
Method for preparing in vivo formulation::Take μL DMSO stock solution, next add μL PEG300, mix and clarify, next addμL Tween 80, mix and clarify, next add μL ddH2O,mix and clarify.
(1) Please be sure that the solution is clear before the addition of next solvent. Dissolution methods like vortex, ultrasound or warming and heat may be used to aid dissolving.
(2) Be sure to add the solvent(s) in order.
CD40-L Blockade for Prevention of Acute Graft-Versus-Host Disease
CTID: NCT03605927
Phase: Phase 1 Status: Completed
Date: 2024-11-27
|
 |
 |